
We knew she was going to be small. After the nurse told me I was 5 cm dilated at 35w 4d, I held Joe’s hand and talked through what was about to happen. Not only would she be much, much smaller than our firstborn was, more than likely we would be heading to the NICU shortly after she arrived.

15 minutes after the anesthesia took hold and they removed her from my stomach, our little Birdie cried and then stopped. She was having trouble breathing on her own, and they quickly whisked her down the hall and into the arms of the NICU nurses on call. Joe followed. I held her little hand a few hours later. What she lacked in size, she made up for in sound. Her lungs were underdeveloped, but her cry let us know she had fight in her.
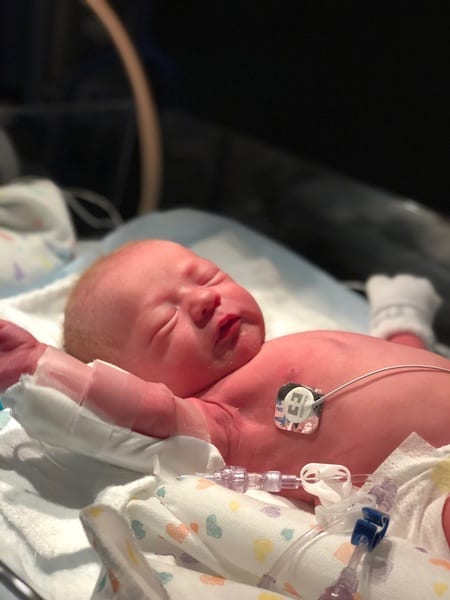

Most babies enter the NICU with issues that threaten their ability to thrive. Their oxygen levels are low. They have trouble breathing. And sometimes, it is a waiting game. Their little bodies still have to develop. And, like so many of the mothers and fathers who have rotated through those doors and down the halls of the NICU, we settled into our room and waited.
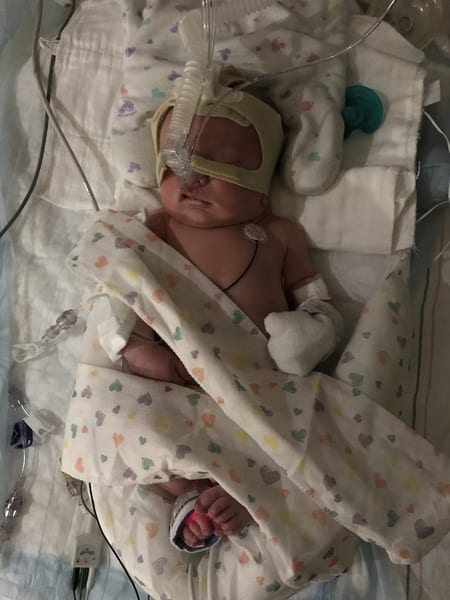

The next 11 days went by in incremental hours of three. There was no day, no night. Only brief moments of rest before and after pump sessions when I waited and waited, waiting for my milk to come in. And while we waited, Birdie was fed donor breast milk in the NICU. As I impatiently waited for my body to do what it was meant to do, I thought about the mothers who carefully packed their gift of donated breast milk, a gift perfectly designed for babies like mine, and I gave thanks. It was the first profound feeling of gratitude I had experienced in the NICU, but it wouldn’t be my last.

After sharing the news that Birdie had been born after a long bedrest and unexpected labor, I didn’t anticipate that the online social community that I had discussed wall decor and sofas with would turn out to be such an anchor of support during my NICU stay. Within minutes of sharing the view from my chair in the NICU, I had messages from mothers and fathers who were currently in the NICU, too, sharing selfies from the exact same seat I found myself in, holding a tiny baby hooked up to at least 10 wires, with the flashing lights and alarms beeping in the background.
It was a club we hoped we’d never have to join, but when you do, you are welcomed with open arms. The vulnerability of having a sick baby, of not being able to be the sole source of support they need, brings a welcoming community of parents who know firsthand how important the help of others is during those extended days and nights.
After we were discharged, my milk came in. I had more than enough to feed Birdie and stock the freezer for my return back to work — something I hoped and dreamed about when I breastfed August. My time in the NICU allowed me to focus solely on producing milk, and that resulted in a gift that allowed me to pay it forward to other families who needed it. I am able to look back at my time breastfeeding as not only giving a gift to Birdie, but also to the other babies who benefited from the milk I was able to donate.

Last month, I donated two freezer loads full of my milk. It is one of the most gratifying things I’ve done, especially because I know what it felt like to not be able to give my baby what she needed most.
Shortly after returning to work, we were introduced to Prolacta Bioscience (who we’ve partnered with on this post). The company was created specifically to provide preemies with human milk-based nutritional products in the NICU when they need them the most. Prolacta is bridging the gap between the benefits that breast milk provides and the extra calories and protein that the very tiniest preemies need. Built on the belief that there is no adequate replacement for human breast milk, Prolacta has created neonatal nutritional products, including human milk fortifiers (HMFs), that are made with 100% human milk, donated by mamas with excess breast milk, to help give preemies the boost they need in the NICU. Prolacta is a privately held, for-profit, and scientifically driven company that is committed to putting its resources and talent behind improving premature infant nutrition and changing the standard of care in the NICU.

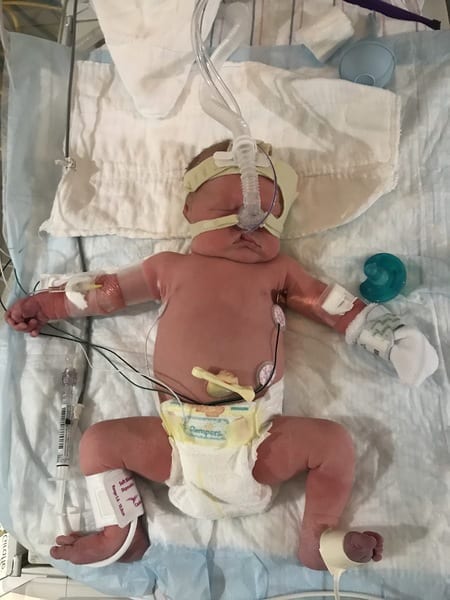
In short, extra-small preemies have a human milk-based option instead of turning to cow milk-based formula or fortifiers. (Disclaimer: For full-term babies, there isn’t anything wrong with formula. I am a proud formula-feeding mama. Both of my kids were switched to formula after my milk stopped at roughly 4 months). Game. changer.
But for preemies, it’s a different story. Cow milk-based nutrition has been shown to increase the risk of serious complications for preemies, including necrotizing enterocolitis (NEC) – one of the leading causes of death for preemies.
So, what exactly do they mean by human milk-based products? Prolacta developed and offers the only HMF derived from 100% human milk, as opposed to other commercial HMFs, which are derived from cow milk. Prolacta’s line of human milk-based fortifiers, Prolact+ H2MF®, provides the tiniest premature infants — those weighing less than 2.2 pounds — with the nutrition necessary to support appropriate growth and development. Adequate nutrition is critical for premature infants in the NICU, who require higher levels of protein and calories than what mother’s or donor milk alone can provide. Check out this infographic to learn more about fortifiers.
When Prolacta invited us to share our NICU story in hopes that it would help raise awareness about the option of Prolacta’s human milk-based fortifiers in the NICU, it was just a no-brainer. If you or someone you know has a preemie, please share this post with them or tag them in the comments below, so they can learn more about the benefits of fortifier made from 100% human milk for their baby.

BY Kate Arends - August 13, 2018
Most-read posts:
Did you know W&D now has a resource library of Printable Art, Templates, Freebies, and more?
take me there
Get Our Best W&D Resources
for designing a life well-lived
Thank you for being here. For being open to enjoying life’s simple pleasures and looking inward to understand yourself, your neighbors, and your fellow humans! I’m looking forward to chatting with you.








The nicu can be such a scary but heartwarming place. Our daughter only needed to be there for monitoring for 30 hours after being born with a severe birth defect (mostly fine, mostly thriving now), but I’ll never remember saying goodbye and giving the most sincere hug of gratitude to the doctor who sent us on our way. I’ll always have a special place in my heart for that doctor.
Paige
http://thehappyflammily.com
My sisters and I are NICU babies. We were born at 30 weeks and all stayed there for a few weeks and as one of us would make progress, my parents would have to balance time between my sisters who got to go home early and then myself who was still in the NICU (we’re quadruplets). My parents were (and are) saints! My sister is now a NICU nurse in the same NICU we were in, coming full circle. Glad Birdie is doing well! 🙂
Thank you for sharing this tender story and these precious photos of such a vulnerable time for you, your family, and your sweet baby girl. I’m so glad she’s now thriving. This makes me wish I was at a stage to donate breast milk. Nursing was one of the favorite things I’ve done in my life. Many blessings to you and your beautiful family, Kate!!
Mimics my story my son born at 33 weeks
Never thought I would think about donar milk but very grateful for it.
Absolutely inspired <3
Thank you for sharing this story. I was a premie (10 weeks early) and NICU baby too. Almost thirty years later, my parents still talk about their time in the hospital with me.
[…] Original source: https://witanddelight.com/2018/08/looking-back-birdies-birth-story/ […]